How is Trauma defined?
The word trauma is Greek in origin and means wound. A traumatizing experience is characterized by the fact that the intensity of the experience, despite stress tolerance, resilience and the available coping strategies and options for action, overwhelms or threatens us existentially to such an extent that we cannot process and synthesize (integrate) the experience. It is not important how extreme the situation is, but how we are able to cope with the stress, thus not every traumatic event causes a traumatic stress response.
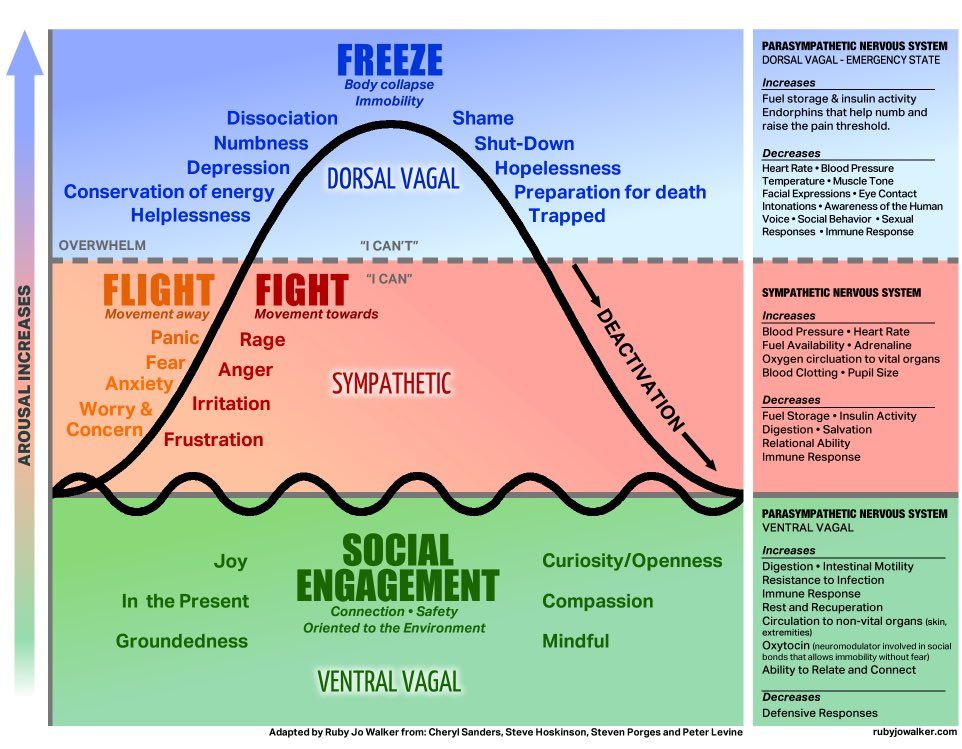
Autonomous Nervous System
Natural reactions to life-threatening situations can be well observed in the animal kingdom. The antelope pursued by the lion instinctively activates the sympathetic part of its autonomic nervous system (fight or flight). Since it cannot win a fight, it chooses flight. If it does not succeed in escaping, the parasympathetic part of its autonomic nervous system takes over body regulation and responds to this life-threatening situation by going from a sympathetic freeze up to a total parasympathetic shut down (slackening and shutting down of all sensory perceptions), which then anesthetizes the animal so it won’t feel the agony of death. If the lion does let go of it – thinking the antelope is already dead – it will jump up at the right moment, flee and once in safety, will immediately shake and shiver. (Engaging self-regulation, stress discharge and a reduction of adrenaline.) By physically discharging what it has experienced, the action is complete for the antelope; it is not traumatized despite this frightening, life-threatening situation.
This natural process shows very well what is often missing in human stress processing in general and in traumatizing experiences in particular – the physical discharge of the stress and regulation of the system, for which especially children need an adult (with a fully developed nervous system), because the child’s nervous system has not yet learned this self-regulation. If the co-regulation by a caregiver is missing, the child develops an insufficient tolerance for stress as well as substitute actions for the failed integration of the experience – traumatic memory becomes an incomplete action. The accumulated, unprocessed stress (trauma) leads to a permanently increased stress level and thus has far-reaching effects on the psyche, health and vegetative system, and often manifests somatically – with muscular tension, a wide variety of physical symptoms (often visceral) and even chronic dis-ease. Substitute actions further deteriorate our individual stress tolerance.
Due to the lack of mental energy, even small challenges quickly trigger a sympathetic (hyperarousal) or parasympathetic (hypoarousal) reaction of the nervous system that is inadequate for the situation and mental processing of the situation is blocked. This contrasts with a healthy person, where the identical challenge can be processed within their individual, healthy stress tolerances and thus becomes easily integrated.
Dissociation Continuum
The trauma spectrum describes the progression from successful to failed processing of stress and overwhelm, beginning with:
- adjustment disorders
- acute stress response
- primary structural dissociation = post-traumatic stress disorder (PTSD)
- secondary structural dissociation = complex traumatic stress disorder (cPTSD)
- up to tertiary structural dissociation = Dissociative Identity Disorder (DIS), in which the affected person distances themselves so strongly from their experience that they can only bear what they have experienced by completely splitting it off (dissociating) and establishing one or more other personality states in its place that carry the experience for them.
Dissociation (the “non-realization” of the traumatization) manifests in different ways and intensities (partial dissociative or complete) within the trauma spectrum:
- de-personalization (lack of personal reference)
- de-realization (dream-like unreality)
- de-somatization (not feeling the body/pain)
- de-affectualization (emotional distance)
- de-temporalization (distorted sense of time).
There may be partial or complete amnesia of the traumatizing experience, brought to consciousness by intrusions, flashbacks, freeze and shutdown experiences, or identity insecurities to the point of identity change (tertiary dissociation), also accompanied by amnesias and/or fugue in the here & now. It is now even discussed whether a large part of psychogenic disorders such as anxiety and obsessive-compulsive disorders, somatization disorders, personality disorders also have their origin in traumatizing experiences.
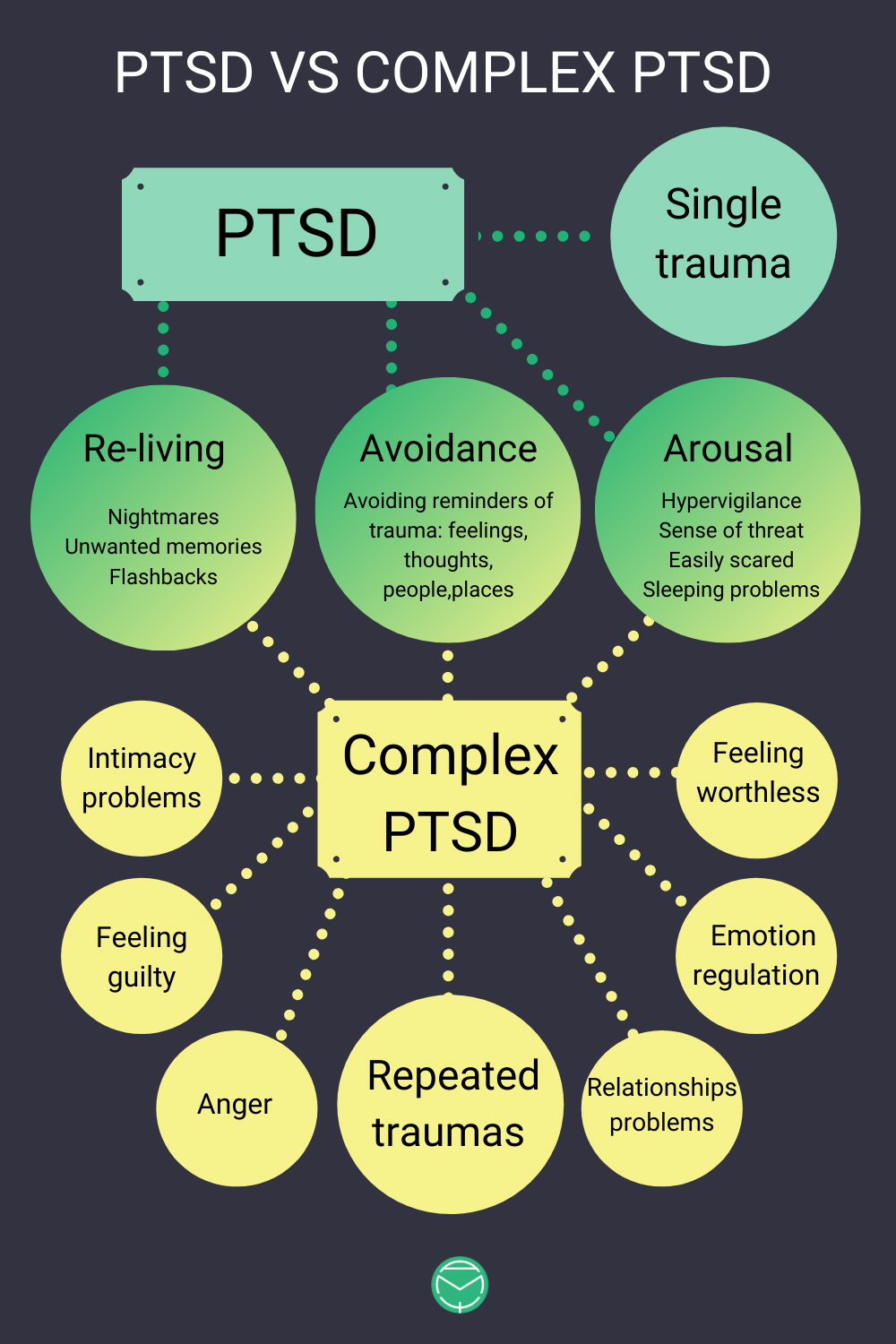
Two Forms of Trauma – PTSD and cPTSD
PTSD triggering experiences include shock traumas such as accidents, war, natural disasters, death, etc. Here the flashbacks and associated panic are particularly frequent.
Developmental trauma (cPTSD) usually originates in childhood and is much more complex and often more subtle. Triggers are e.g. emotional neglect, devaluation, violence, abuse, etc., which are mainly characterized by the repetitions that create enormous stress for the helpless child; being is dependent on the caregivers, they don’t have the possibility to fight off these situations or to escape (fight or flight). In this process, the child is caught in the ambivalence between attachment and love for their caregivers and the fear and terror generated by the traumatizing experiences.
Therefore, the survival strategy is a partial or complete dissociation of the traumatizing experience and identification with the aggressor through internalization of the threat and formation of an ego-dystonic introject (guilty processing, internalized voice). In this way, attachment (survival) and thus a superficial, coherent integrity with oneself and the aggressor can be maintained, as the natural, instinctive reactions to life-threatening situations are not available to the child in his dependence on the aggressor. The transition to tertiary dissociation is fluid and dependent on the intensity of the experience; this occurs primarily in victims of organized (sexualized) violence.
Dissociation and introject formation are therefore vital protective mechanisms for the helpless child, however are no longer adequate or necessary in adult life. Maintaining them requires enormous mental energy, which has symptomatic effects ranging from exhaustion, intrusions and flashbacks of the traumatizing experience to the disintegration of the ego identity and can lead to the affected person no longer being able to lead a normal life as the pressure of suffering is very pronounced. Traumatic experiences thus have a massive impact on the organization of the nervous system and the internal system, which is why trauma sequela are also considered a physiological disease, since the effects at the mental and action-based level cannot be controlled by the person at will. The nervous system, which is programmed and sensitized to alarm, receives a triggering stimulus and the rehearsed and neuronally-linked response pattern runs automatically and is experienced as ego-dystonic and externally determined.
The first steps to restructure the nervous system are resource work, which focuses on the person’s strengths and abilities as a counterbalance to the stressful experiences. This strengthens mental energy, and a supportive, compassionate, and safety-giving environment that allows dwelling in the ventral-vagal attachment mode. Identifying external resources and attachment figures to draw upon is also an important step. Through this focus, new neural pathways can be linked and reinforced through repetition, which in the future will help the person in challenging situations to activate step by step a more adequate vegetative response strategy and to stabilize further and further.
As with everything that is newly learned, it takes patience to establish these previously non-existent or barely existing neural connections. Therapeutic methods in the stabilization phase are e.g. resource, joy or gratitude diary, mindfulness exercises, imagination of a safe place, inner strengths conference, practicing dealing with flashbacks and freeze.
How the Inner System works in Trauma Therapy
As soon as the system is sufficiently stabilized, the traumatic material begins to show itself, as it wants to be integrated. In trauma therapy, therefore, much work is done with the imagination and hypno-therapeutic methods, which make it possible to get to know and restructure the inner map and organization of the personality. First of all, it is about compassionate and caring witnessing of one’s hurt parts, recognizing and acknowledging the protective mechanisms once created as necessary for survival and becoming aware of the temporal discrepancy (here&now vs. there&then).
Through the preparatory imagination and observer perspective exercises, contact is made with the inner world. It is perceived that there is still someone inside who can observe everything – the ego-syntonic ego-states (willingly accessible parts of the self, e.g. our roles in family, work, friendship, public) are learned to know and distinguish, and the perception and impact of feelings and thoughts are sharpened. This preparation is essential for the challenging phase of trauma confrontation, in which the dissociated, wounded inner parts are also invited to show themselves in their existential need through various imagination exercises.
These wounded or fragile parts are trapped in the traumatizing experience. They hold for us, so to speak, the experience that we had to split off there&then in order to survive. They are usually protected by an ego-dystonic part, which ensures our survival (control) and fights (outbursts of rage, aggression, violence, perpetrator introspection) in case of danger (trigger) and thus tries to prevent the triggered, fragile part from overwhelming us with its feelings (intrusion).
According to Richard Schwarz and his approach of the Internal Family System (IFS), it is necessary to first obtain the permission of the protector part in order to make contact with the injured or fragile part. As soon as the fragile part is emotionally witnessed and released from the traumatic situation, the protective part can take on a new task in the internal system. Often these protector parts are particularly powerful, talented, creative, etc. parts. Their abilities were not available to the system until then because of their protective role. A third variant of a traumatized part is fixated on attachment and often expresses itself as a “people pleaser”, e.g. in the form of difficulties with demarcation and saying no, an exaggerated need for recognition and a lack of self-worth.

How we finally heal from trauma
The challenge now is to overcome our fear of the feelings and memories of the hurt parts and, with the support of a safe and stable environment, to find the courage to witness and allow these feelings and memories so that they can be integrated into the inner system. Typical avoidance strategies are excessive preoccupation (workaholic), substance abuse, emotional withdrawal, attachment avoidance, blaming others, rationalization, etc. (see S. Freud defense mechanisms). In this way we can maintain our everyday functions and do not have to face what we have experienced.
Dissociation is a substitute action for the integration that could not (yet) take place (completion of the action). In therapy, contact is made with the injured and fragile parts in a very gentle and slow way, step by step, making sure that we are well emotionally stabilized to engage in this venture in order to prevent re-traumatization.
One method is the inner conference – an imagination exercise in which we identify a negative belief set that is essential for us, turn it into a positive one, and thus invite the inner conference of all parts that want to express themselves. Usually, those parts for which this positive statement does not apply then show up, giving us the opportunity to witness and feel the feelings and ideas of these parts, thereby releasing them and freeing them from their role.
Once we have synthesized (realized, personified and presented) the traumatic memory, the action is complete.


